By Anna Betz for Enlivening Edge Magazine
Part 2 (Part 1 is here.)
Why Self-management for a Public Health Service like the NHS?
Imagine health or social care organisations where staff and citizens are interested in optimising each other’s health and wellbeing. What if they discover what gets them out of bed in the morning, and start co-creating the conditions where everyone can flourish? The community projects described in Part 1 of this article are a great start, and to move further we must turn our attention back to transform the organisations themselves.
The operating system and organisational processes that align with this approach to health creation are self-managing. If we work to enable citizens to be independent and responsible for their own health, we should align our approach to staff in a similar way.
 We must support our staff to be accountable for their own work, expect them to make best use of their talents and skills and to promote their own wellbeing. We must trust them to make great decisions that support our citizens.
We must support our staff to be accountable for their own work, expect them to make best use of their talents and skills and to promote their own wellbeing. We must trust them to make great decisions that support our citizens.
Staff able to do this will be confident they are making a difference, be happy and healthy individuals in our communities, and feel valued and motivated in their work. Our organisations, like our communities, will sense and respond to what is needed, developing agility by decentralising decision-making and control of resources.
 We think the way we just described of organising and supporting people and communities to be health-generating is congruent with NHS (UK National Health Service) values. In the NHS we talk often about compassionate care, and compassionate leadership and organisations.
We think the way we just described of organising and supporting people and communities to be health-generating is congruent with NHS (UK National Health Service) values. In the NHS we talk often about compassionate care, and compassionate leadership and organisations.
Aligning these approaches offers a real opportunity to realise all this. Indeed, self-compassion and compassionate conversations will be the way to achieve the behaviour change which the success of this care model depends upon.
Finally, if, as we are told, the NHS is in crisis, then we could ask what investment is required to achieve the quality of outcome we aspire to? Buurtzorg famously demonstrates a significant reduction in management and back office cost compared to traditionally managed nursing and care providers. If we are prepared to make this change, we could take these potential savings and reinvest them in ways that add the most value for our citizens and communities. Is this the ethical and logical path? If so, what do we know and what can we do that can help this to happen?
Successes and challenges of strength-based approaches, co-production of health and self-management in the NHS
Buurtzorg Britain & Ireland
 In December 2017, at RSA House in London, Jos de Blok helped launch Buurtzorg Britain & Ireland. For the last couple of years, he has worked in partnership with the social enterprise Public World. They have been supporting nurses and support-workers, and employers, to apply the lessons of their experience in the NHS and social care all over England and Scotland. According to Jos “it is still early days, but the signs are promising, as shown by an independent evaluation of the neighbourhood nursing teams in the London boroughs of Lambeth and Southwark published in January 2018.
In December 2017, at RSA House in London, Jos de Blok helped launch Buurtzorg Britain & Ireland. For the last couple of years, he has worked in partnership with the social enterprise Public World. They have been supporting nurses and support-workers, and employers, to apply the lessons of their experience in the NHS and social care all over England and Scotland. According to Jos “it is still early days, but the signs are promising, as shown by an independent evaluation of the neighbourhood nursing teams in the London boroughs of Lambeth and Southwark published in January 2018.

“This [Buurtzorg] model of community home nursing offers real potential for addressing some of the challenging issues facing patients, carers. and nursing staff,” Professor Vari Drennan MBE said.
According to Brendan Martin, Managing Director at Buurtzorg Britain & Ireland and Public World, self-management of teams themselves has been the relatively easy part. He says “the challenge now is to repurpose institutions and organisations to provide necessary supports institutions and organisations to provide necessary supports very well and stop doing useless things”.
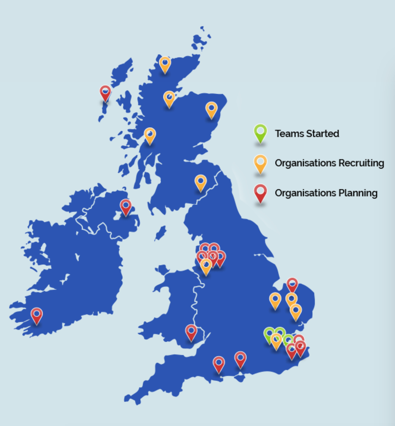
Whether Buurtzorg-style Buurtzorg-style healthcare works in the UK depends on whether or not system leaders and organisational leaders rise to their part of the challenge as well as the frontline teams are rising to theirs.
Buurtzorg’s experience of supporting transformation of other Dutch providers has shown that radical overhaul of managerial and administrative arrangements to produce agile and lean service centres is a key success factor.
Models of collaboration and of co-production of health in the UK public health service
Lambeth GP Food COOP – a community-led health cooperative within a GP practice

Operating in London, it is one of the first community-led health co-operatives working in and for the NHS. Since 2013 they have built gardens in GP surgeries designed to support patients with long-term health conditions to learn how to grow food and, by doing so, improve their health and wellbeing.

Bromley by Bow Health Centre (BBBC)
It is another example of a GP practice that uses a strength-based approach in partnership with the community. BBBC incorporated a GP practice 20 years ago as an integral part of the model they were building, and rented it back to the NHS. BBBC embodies many of the principles behind the idea of the commons. They took ownership of a 3-acre park which had been neglected. They persuaded the local authority to give it to them on a 30-year lease. The same happened with the GP practice. They thought they could do a better job than the NHS were doing at the time.
The passions of the local community, with creativity, self-expression, co-production, and an “asset-based” approach have been at the heart of the project since the beginning.
Programmes are conventionally funded. Models about healthy living are brought into everything. Working with people in a different way which includes social prescribing and the ‘intelligent waiting room’, an idea to use the waiting room as an engagement space.
BBBC is a “knowledge share” programme. 1500 people have come from all over the world to participate in it. The usual way of looking at patients is looking at their problems—what’s wrong with them and things that need fixing—whereas “asset-based” working looks at the positives, and is using a catalyst to bring people together. Of course resources are needed to manage these assets, and BBBC is keen to create structures for that and to support others in doing so.
 Conclusion
Conclusion
Having learnt about the successes and challenges of Buurtzorg Britain & Ireland, Lambeth GP food cooperative, the Bromley by Bow Health Centre, and other projects co-produced by the NHS and the community, how would you respond to consultants working in this field claiming that Self-Management in the NHS was attempting the impossible and that large public organisations like the NHS could never make this move?
What could self-management if applied to the whole of the NHS as a public service look like?
Join the conversation and help us to figure it out together by joining us at the IEC conference, by commenting on this article and/or by sending a message to Anna at [email protected].
“Let’s be realist and go for the impossible” as the French students said in May 1968!
Anna Betz, Jane Pightling, and Helen Sanderson will be co-facilitating workshops at the IEC Conference. We look forward to your support to sense into where this journey needs to take us next.
If you are curious about the part you can play in re-inventing health and social care, why not register for the IEC2018 conference and join our workshops on Friday 25th May. When you register to join the conference following this link don’t forget to mention that you are interested in the Teal Org Track.
References:
Can we radically transform the way we deliver health and social care in the UK? By Brendan Martin (RSA blog)
Building a Global Movement for Patient Centred Care, by Jos de Blok (RSA blog)
Featured Image used by permission.
 Anna’s background is in Health and Social Care with training in Herbal Medicine, Socialwork, Mindfulness Practice, Transparent Communication, and Systemic Family Therapy. She practices a pro-active evolutionary approach to Health and Wellbeing and leads on projects in the UK National Health Service using Mindfulness and diet for people suffering from chronic inflammatory diseases like diabetes and dementia. Her passion for building thriving and sustainable communities inspired her to co-found the HealthCommonsHub. She feels at home in places where individual, communal, organisational, and social evolution meet, and where people support each other in becoming whole and feel enlivened.
Anna’s background is in Health and Social Care with training in Herbal Medicine, Socialwork, Mindfulness Practice, Transparent Communication, and Systemic Family Therapy. She practices a pro-active evolutionary approach to Health and Wellbeing and leads on projects in the UK National Health Service using Mindfulness and diet for people suffering from chronic inflammatory diseases like diabetes and dementia. Her passion for building thriving and sustainable communities inspired her to co-found the HealthCommonsHub. She feels at home in places where individual, communal, organisational, and social evolution meet, and where people support each other in becoming whole and feel enlivened.