By Anna Betz for Enlivening Edge
Reflection on the NHS Employers Summit 2015
Talking about our vision for healthcare is the necessary yet the easy part. Walking the talk requires much more: a shift in perspective.
There is a large gap between the wonderful ideas and aspirations I heard leaders express at the recent NHS Employers Autumn Workforce Summit 2015, and the present reality of NHS policies, structures, and procedures. It’s so large a gap that it might almost seem paralyzing. That is, if you’re not aware that another way of doing healthcare is not only possible, but is already happening in a few isolated places. You’ll find a number of them discussed in my article on “The future of our NHS and the power of community.”
What seems to be missing so far is their knowing about each other, and creating intentional collaborations to discover their collective intelligence and impact on building a different kind of future.
As I sat in the audience, listening to some of the honest observations offered by the NHS leaders on the Summit 2015 panel, on one hand I heard and shared their heartfelt desires for the future of healthcare, and on the other hand, I also sensed their feeling of stuckness.
I could sense potentially transformative energy moving within our old, crystalised structures, and I felt privileged to silently bear witness to an evolutionary impulse, a creative force of innovation, wanting to work itself through people in an area I had previously not expected it to emerge within.
Whether such meetings will help to revitalize our NHS will depend not only on the leaders, but on all of us who are working as a co-creative and collaborative force, a social movement for better healthcare.
Leaders alone, no matter how visionary they are, cannot rescue a broken system. What they can do is to inspire and catalyse a social movement, connect with it, and listen to its heartbeat.
 My hope is that some leaders will understand this and will help create environments favorable to self-organization, where this innovative and revitalizing energy can move freely without having to report to a command-and-control management structure.
My hope is that some leaders will understand this and will help create environments favorable to self-organization, where this innovative and revitalizing energy can move freely without having to report to a command-and-control management structure.
I don’t believe goals like creating a positive culture and greater staff retainment, and practising compassion, collaboration, trust, and connectedness, can be imposed or created by leadership from the top down. These are qualities, competencies, and skills that typically develop and flourish in spaces that are outside of management control, and not all of them can be readily measured by performance targets.
The Summit panelists weren’t short of offering wonderful suggestions how to reach these goals. However, I didn’t detect a collective will to actually identify practical ways of realising them.
I couldn’t help being reminded of why I attended this Summit in the first place, which was to take part in a workshop with Jos de Blok, the founder of Buurtzorg, a forward-thinking home health care organisation in the Netherlands. Buurtzorg is a working example that puts suggestions such as those discussed at the Summit and mentioned below, into practice, with outcomes we can only dream of in the NHS.
- Develop practices based on the realisation that healing comes from feeling connected and having a purpose and that everyone has something valuable to contribute if encouraged to do so.
- Train professionals to be good communicators and good listeners – professionals who can enable participation, networking, and collaboration so that everyone can feel empowered.
- Harness the talent of everyone; allow and support nurses to initiate and lead projects.
- Decrease bureaucracy.
- Have a skill mix in teams; think of the bigger picture rather than focusing only on one’s own limited professional identity; bring decisions back to local teams and employ local experienced people who understand the cultural context of patients; support professional judgment rather than confer responsibility to clinical experts for work that other professionals can do.
- Use the best available information and communication technologies to support community services.
- Integrate Human Resource folks rather than their working in an ivory tower. HR professionals should model good behavior and bring this to organisations.
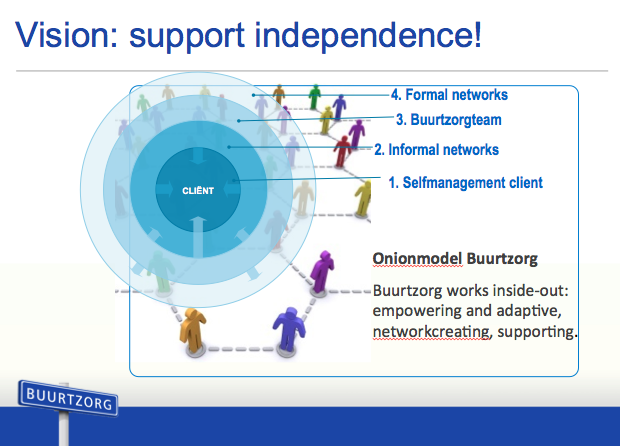
What Jos de Blok demonstrates with Buurtzorg, and the message that resonates with me strongly, is that by trusting human beings to sense and co-create what wants to happen in a health ecosystem (which includes nurses, patients, and their communities,) miracles can happen. As the CEO, Jos has created spaces for both nurses and patients to flourish in an interconnected network where mutually-supportive relationships are enablers of health. Buurtzorg’s self-managing governance practice absorbs complexity without creating a bureaucratic management structure around it.
According to Jos, the most important factor that makes this lack of bureaucracy possible is trust: in ourselves, in each other, and in our shared purpose. Cepta Hamm, Head of Nursing, Adult Community Services from Guy’s and St.Thomas NHS Foundation Trust had this to say after visiting Buurtzorg herself: “I am no longer worried about the clinical aspect of the model. The challenge will be in creating the space for the teams to flourish.”
Every team in Buurtzorg is connected to every other team via an online platform whilst being autonomous enough and small enough to serve the needs of every nurse and every patient in their area. Buurtzorg teams are living proof that working as an interconnected network of autonomous cells optimizes the potential of everyone and saves a lot resources, financial ones included.
Buurtzorg is responding to an increasingly global and complex world, with simplicity-beyond-complexity, common sense, and clarity of purpose, not by creating a collection of separate organisations but by fostering the emergence of a powerful nervous system of nodes of small diverse teams which are trained and supported well enough to respond to their challenges without orders from above.
Every nurse in this network has the potential to create and hold their own vision — to unfold their own calling in life. They can all build relationships and connections, ask for help and support, so that they can bring their vision to life.
Buurtzorg operates in the context of the insurance-based healthcare system in the Netherlands; thus, some of its structural aspects are not directly transferable to the UK’s NHS. It is nevertheless one of the pioneers of “the most important trends of the 21st century which is going to take us out of the 20th century institutional world and moving towards a post ‘employment’ model of making a livelihood, into a post-capital-centric model of entrepreneurship, towards sharing, community and family, out of the cult of consumerism, towards unschooling, lifelong learning and, perhaps most importantly towards ‘spirituality’ in the sense of personal and societal values and purpose development.” (Victor Vorski)
My hope is now that some forward-thinking leaders from gatherings like this Summit, and some workers from the frontline – some of whom made the RCN event with Jos de Blok in July such a success – will find ways to connect soon and start together energizing a movement in the UK, a movement which so far remains rather disconnected.
As a certified NHS Health and Care Radical, I am in support of Helen Bevan when she says that “there needs to be a shift from ‘change programmes’ (designed by leaders) to ‘change platforms’ (where leaders, workers, and citizens connect and collaborate) in the NHS, if change is ever to become a new norm.”
If you feel drawn to help the NHS getting unstuck, whether you are in a leader position, work on the frontline with patients or if you are a citizen, I’d like to connect with you. Please post your comments/questions below or drop me a line at anna(at)schoolofcommoning(dot)com.
NHS Employers Autumn Workforce Summit 2015 Exploring solutions to your long term workforce challengesPanel Chair: Daniel Mortimer, Chief Executive, NHS Employers · Jane Cummings, Chief Nursing Officer for England · Professor Sue Hill, Chief Scientific Officer · Suzanne Rastrick, Chief Allied Health Professions Officer · Hugo Mascie-Taylor, Medical Director, Monitor
In her blog ‘Going Dutch’ Kate Ling, senior policy manager leading on workforce issues at the NHS European Office, reflects whether Buurtzorg, or something like it, can be replicated in the English health system, which is very different from the Dutch.
 Anna’s background is in Health and Socialcare with training in Herbal Medicine, Socialwork, Mindfulness Practice, Transparent Communication and Systemic Family Therapy. She practices a proactive evolutionary approach to Health and Wellbeing and leads on projects in the NHS using Mindfulness and diet for people suffering from chronic inflammatory diseases like diabetes and dementia. Her passion for building thriving and sustainable communities inspired her to co-found the HealthCommonsHub. She feels at home in places where individual, communal, organisational, and social evolution meet and where people support each other in becoming whole.
Anna’s background is in Health and Socialcare with training in Herbal Medicine, Socialwork, Mindfulness Practice, Transparent Communication and Systemic Family Therapy. She practices a proactive evolutionary approach to Health and Wellbeing and leads on projects in the NHS using Mindfulness and diet for people suffering from chronic inflammatory diseases like diabetes and dementia. Her passion for building thriving and sustainable communities inspired her to co-found the HealthCommonsHub. She feels at home in places where individual, communal, organisational, and social evolution meet and where people support each other in becoming whole.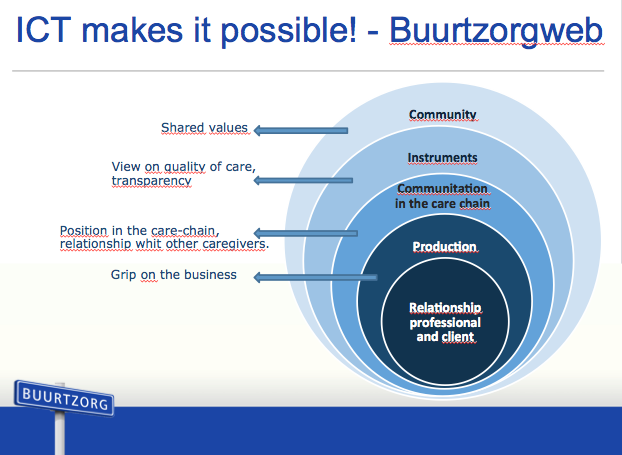



Anna I am totally drawn to helping the NHS get unstuck and would love to connect – I used to be a nurse feel like the NHS is my source point even tho I haven’t worked in it for years. A recent spell in hospital was like a massive wake up call for me. Im speaking to people here in the North of UK about how to open spaces of dialogue around transformation – please be in touch so we can share whats up. [email protected] or 07947507382 Linda xx
Dear Linda,
Thank you for responding to your wake up call and reaching out. “To open spaces of dialogue around transformation (personal and organisational) everywhere” is exactly what we need. Do you have any particular area/group/location in mind where you would like to explore possibilities? Where do you live in the North and do you know other people who may resonate with your intention? My e-mail address: [email protected]
Dear Anna,
yes we need new ways of working would like to connect up at some point to move the possibilities forward ! Bill
Dear Bill,
I would love to connect with you and discuss further. My e-mail: [email protected] or mob: 07731584358
Hi Anna
I really enjoyed reading your blog, thank you. I too feel this gap and sense of fog as in in not seeing the way forward. You have shared some great examples of how we can have a different way ahead of us somewhere but I also see and feel other people recognising the gap/fog in front of us. It will take a huge amount of of courage from a lot of leaders to bring ourselves to the same space where we can collectively discover the way through the fog.
Dear Angela,
I agree it will take a huge amount of courage from leaders, doctors and other health professionals as well as patients to step out of our habitual comfort zone and maybe dare to say things that may not be so popular in a consumer culture.
We tend to continue perpetuating old habits just because we get so used to them even when they no longer serve us well. Also many health professionals feel they dont have enough time or mind space to learn and think in different ways. After all we get paid to keep the system running as it is and challenging it constructively takes courage. I know from experience how difficult it is to step out of routine and be creative while working in the system.
There is also the added tension of how to keep the NHS public and free at point of access while helping patients to become less dependent on it through providing more empowering education, help them change from being consumers and overuse a shared public resource like the NHS to co-creators of health.
A number of things need to change to bridge the gap and lift the fog, i.e. our attitude and behaviour towards our health through becoming more proactive and responsible in our health behaviours and model this for our patients.
We need to change our mindsets and behaviours from being prescribers of drugs to also become health facilitators. Dr. Rangan Chatterjee demonstrates this so powerfully in the series ‘Doctors in the House’ on BBC1. the documentary is running at the moment (see link at bottom) and well worth watching on Wednesday evenings at 9pm. It shows us the kind of people skills needed in addition to understanding health from a more systemic perspective.
Dr.Chatterjee example could encourage his colleagues not to be afraid to challenge patients attitudes and behaviours while walking compassionately alongside them in their pain and taking the time to do so. Dr.Chatterjee’s intervention radically changed the health of a whole family in a very short time, saves a huge amount of resources long term and makes everyone feel more enlivened. A win win for everyone including the doctor who admitted to feeling more satisfied when he could make an actual tangible real difference to his patients.
Patients are actually the most important overlooked renewable resource in healthcare and healthcare professionals need to be able to access this resource by helping to make patients discover their own potential and feel empowered. What wasnt mentioned in the programme is that Dr.Chatterjee practices a systemic approach known as Functional Medicine. In my role as a herbalist, I also practise a form of systemic medicine known as Endobiogeny http://www.unleashourhealth.com/endobiogenics.html. In Lithuania there is presently a training programme for doctors in Endobiogenic medicine which enables them to apply their existing knowledge and skills in a more systemic way. It also teaches them when and how to use dietary and lifestyle approaches as well as natural medicines made from plants to treat root causes rather than symptoms.
Coming back to changing the system, we need to put more power back into the hands and hearts of professionals, front line workers and patients by creating a healthcare system that encourages creativity, self-care and preventative healthcare.
Our present command and control structures leave little space and opportunity for that. I am continuously leaning into this tension in my work looking for ways of opening up the old crystalised system and help patients to feel more empowered and in control of their health. Do get in touch if you would like to discuss further.
http://www.bbc.co.uk/mediacentre/proginfo/2015/46/doctor-in-the-house